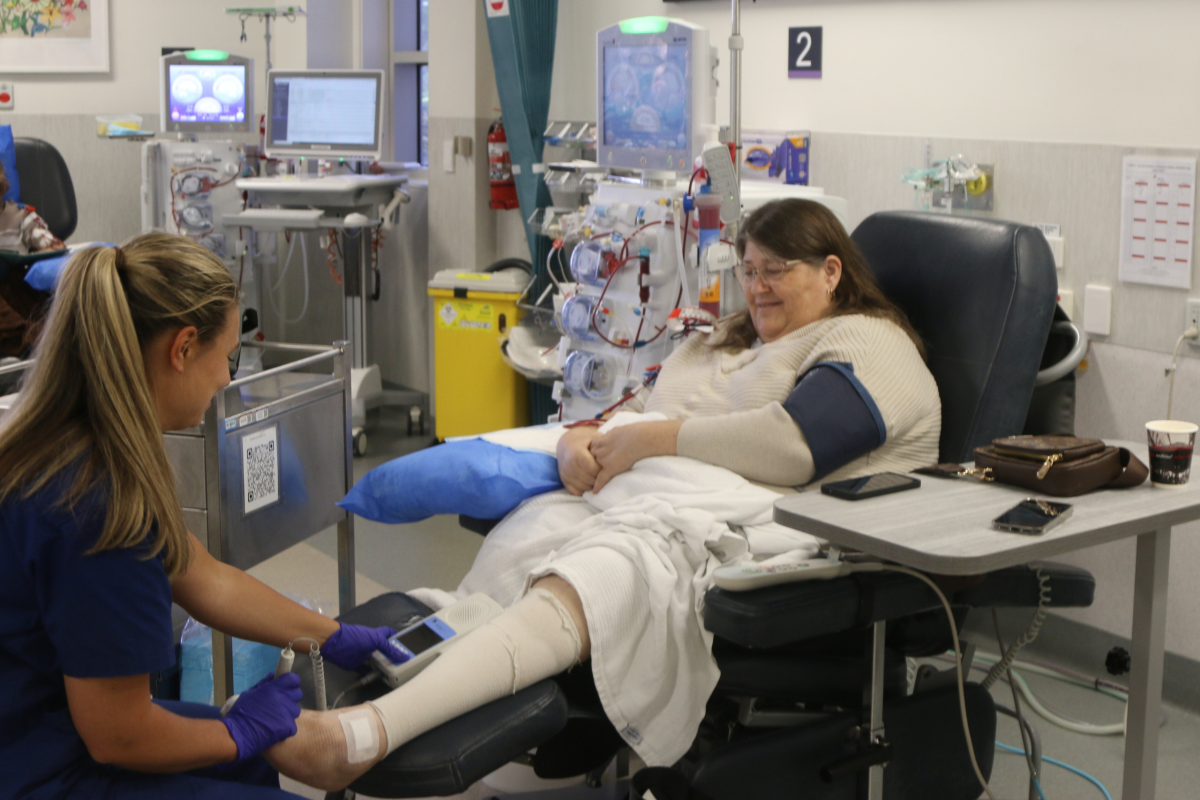
With over 100 participants, Bayside Health Peninsula operates a full time renal podiatry program, which is the largest in the state.
“It’s more proactive and also more responsive,” says Head of Podiatry & Orthotics Elise Gillies, who first wrote the business case for renal podiatry service back in 2022.
“Consumers in the dialysis unit usually come three times a week for up to five hours per session where they are sitting attached to their dialysis machine, and that reduces their ability to get out and about to appointments,” Elise explains. “So the goal of introducing the service was to bring the care to them when they’re here to make our service more accessible for those consumers.”
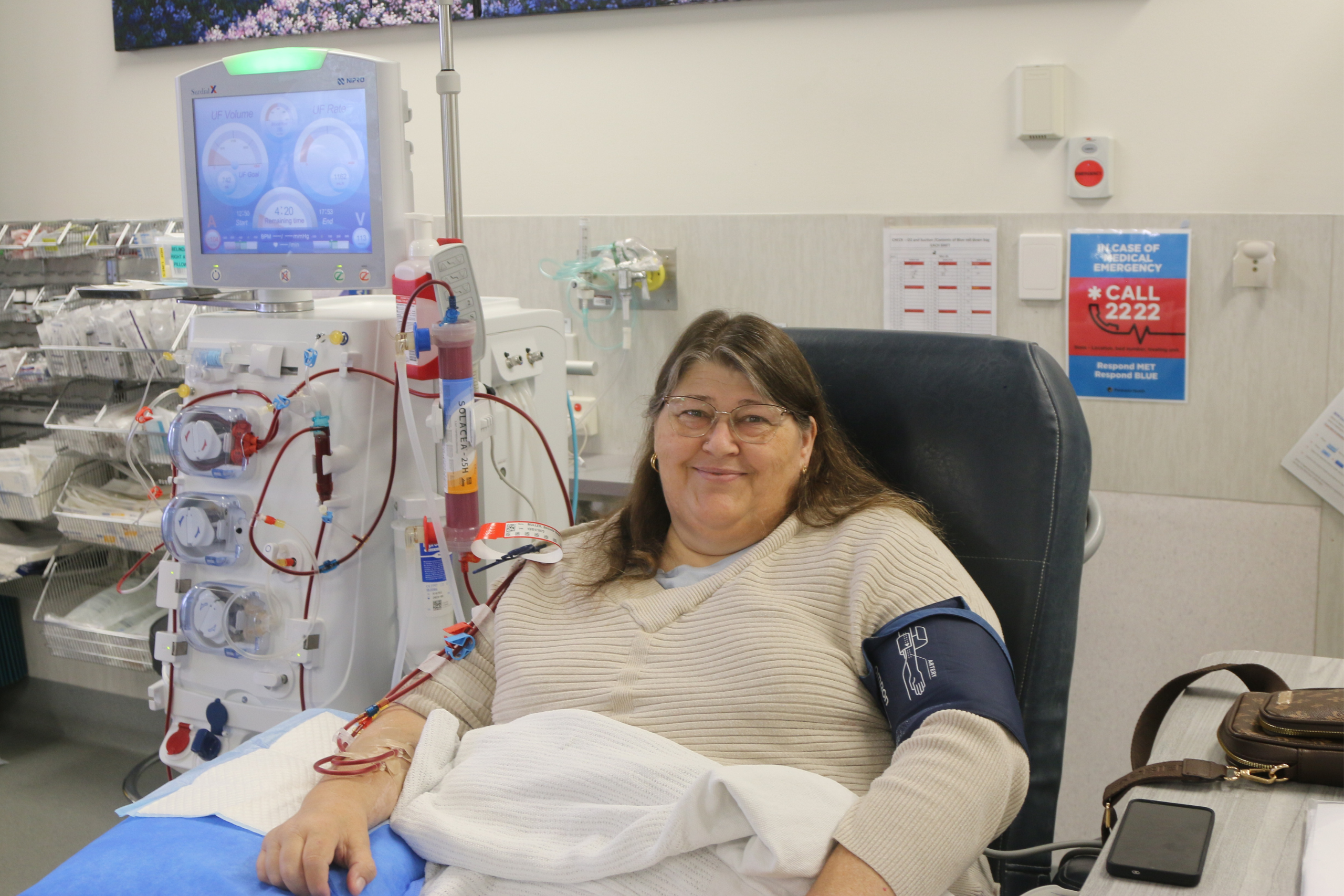
For people like Belinda Muller, doubling up on a podiatrist consultation during dialysis treatment is more than just a time-saving convenience. It also enables her to continue working part-time, despite a complicated treatment schedule.
“It means that I’m not having to come to the hospital every day of the week,” Belinda says. “Because people have a life as well. When I’ve got the convenience of having something happen when I’m sitting in a chair anyway, having that option is so much better.”
Belinda has had an above the knee amputation and manages several chronic health conditions. However she’s a firm believer in making the most of life, and keeping on top of your health – and the renal podiatry service is a big part of that.
“Them coming and making sure my wounds are okay each week means I’m reducing the risk of having to have another amputation,” Belinda says. “Because you can really keep an eye on how you are.”
Senior podiatrist Georgia Filosa, who previously worked within the renal podiatry service, sees patients across all Bayside Health Peninsula’s hospitals and community health sites, and says that the clinic is especially beneficial to patients who might be unable to get a GP appointment, or could otherwise be waiting up to six weeks to see a private podiatrist.
“We have such a good relationship with the nurse practitioners and the endocrinologists in dialysis that in the situations where patients are needing antibiotic therapy, that we can coordinate that without needing the patient to physically attend their GP, which would save the patient so much time and money,” Georgia says.
Camilla Phillips is the High Risk Foot Clinic Coordinator and senior podiatrist who also previously worked within the renal podiatry service.
“Patients undergoing dialysis are at a high risk of developing foot complications and wounds,” explains Camilla. “By providing podiatry care within dialysis allows these issues to be identified and addressed early, enabling preventative strategies that can help improve patient outcomes.”
“The escalation process from dialysis is really smooth in that if we do notice something that we are concerned about, we’ve got people around us that we can escalate to straight away,” she says.
Another innovation of the service was the recognition that foot complications, especially for those consumers with renal disease and diabetes, were often caused by ill-fitting footwear.
“We have capacity to support a pair of shoes for every dialysis consumer so that we are able to fit them with a pair of shoes which fits well and aims to prevent foot complications, again, on the preventative side,” says Elise.